Physics Lessons Applied to Health
During my first physics course in college, my professor told the class (I’m paraphrasing), “the most compelling part of my field of study is investigating the causal mechanisms that lead to observable change.” For example, a satellite attached to a rocket in a storage area at Cape Canaveral would not be demonstrating interesting physics, but the same satellite orbiting the planet would be displaying more complex physics. However, satellites in orbit move within a predictable curved path around Earth, which is easily calculable by a competent physicist. Compared to the previous two scenarios, what is far more interesting for physicists, and far more challenging, is understanding how to get that satellite off of Earth’s surface and into Earth’s orbit. There is an immense amount of change within that transition, and therefore an immense amount of problems to solve. So many problems it’s not uncommon to witness the world’s best unintended fireworks when watching an unmanned satellite mission attempt to escape Earth’s atmosphere.
The essence of my professor's message was, “Notice where there is change, and investigate what is happening around that change. What causes change, and what stops change?” There are valuable parallels that can be drawn from this physics perspective to better understand human health, both in how diseases manifest, and how we experience, or fail to experience, impaired function. This article will focus on the latter: how an appreciation of physics provides helpful insights in understanding our own perception of health.
Let’s start by taking a look at plane travel and sleep deprivation. You’re likely already making obvious and relatable connections between airplanes and lack of sleep. Such as, getting up when it’s still dark out to make sure you’re able to be at the gate for your early morning international flight. Or, not being able to sleep on a redeye because of crying babies, turbulence, or cramped economy seats. However, I’m not referring to a literal connection between plane travel and sleep deprivation, but a conceptual parallel.
Consider what it’s like to be on a plane. Barring extremely rare mid-flight calamities, when do you physically feel the movement of the aircraft the most? It’s always during take off and landing because this is when the plane's speed goes through the greatest amount of change (i.e. acceleration). When at cruising altitude, the plane’s speed is actually about three times that of the maximal take off speed. However, cruising, by definition, denotes a constant speed in a near-constant direction (there is not a whole lot of change occurring). A plane sitting still on the tarmac feels just about the same as when you’re flying over the Midwest during a coast-to-coast flight, except that your seat is vibrating.
As the plane drastically slows down during landing, you’re in the next most physically perceptible phase of the flight. The key insight here is that the maximal speed of the plane is far less physically perceptible than the rate of change in speed of the plane. The greater the change in speed, and the shorter amount of time the speed change occurs within, the more the human body perceives that change. One will always feel acceleration more than maximal speed, if maximal speed is constant. If this inspires skepticism, consider that Earth moves at about 67,000 mph along its heliocentric orbit while simultaneously rotating along its axis at about 1,000 mph. Boiling this concept down even further to our own experience of health, simply remember: change is more perceptible than magnitude. Next, I’ll illustrate practical examples, bringing back the previous mention of sleep, and lack thereof, but in a different light.
Change is not only more compelling than constants in an intellectual sense, as posited by my physics professor, it’s also more compelling for our body’s sensory systems and cognitive self-perception. Our bodies and minds are evolved to be more attuned to changes rather than constants. Consider how you lose sense of your body, your surrounding environment, and your own thoughts, as you lie down to allow sleep to happen. This loss of attunement to the body, environment, and mind occurs because you’re in a stable environment with little to no change/stimuli.
I remember sleeping in a camper trailer out in the Sonoran desert during one summer, and the bed was above a very loud, heavily-vibrating swamp cooler. I was worried I would be kept up all night by the noise. However, since the humming and vibrating occurred in a constant pattern, the swamp cooler was essentially a giant white noise machine. Not only did it not keep me up, it actually woke me up when it randomly turned off in the middle of one night. The sudden loss (change) in noise is what roused my senses. Remember, “change is more perceptible than magnitude”. Less noise doesn’t necessarily mean more peaceful sleep when the existing noise is smoothly constant and suddenly drops away.
The previous example illustrates how our sensory systems are more attuned to change rather than constants, and now I’ll provide an example of how our own self-perception is the same way, for better or for worse. I’ll continue with the theme of sleep. In a 2003 study by Van Dongen et al., the researchers found [1]:
Poor sleep leads to impairments in psychomotor vigilance and cognitive function. Psychomotor vigilance refers to the ability to respond to a sudden situation or changing environment with voluntary, coordinated movement, like driving a car safely or being able to dodge an unexpected object coming at you. Cognitive function refers to the ability to think clearly and do problem solving.
Chronic sleep deprivation leads to a progressive, gradual decline in psychomotor vigilance and cognitive function. This gradual decline continues for at least 2 weeks during continual sleep deprivation.
Individuals who go from sleeping well to sleeping poorly (i.e. 6 or less hours per night) are initially able to accurately self-rate their own deficiencies in psychomotor vigilance and cognitive function (i.e. they know these abilities are negatively impacted by the lack of sleep).
Individuals who chronically sleep poorly lose the ability to accurately self-rate their deficiencies in psychomotor vigilance and cognitive function. This means the level of actual performance impairment increases, but over time, sleep-deprived humans think they’re performing just fine.
To sum up the process outlined above: we don’t adapt to sleep deprivation, but we think we do. This inability to accurately perceive our own fatigue-induced shortcomings is quite insidious considering fatal car accidents due to sleep deprivation occur at a similar or greater rate than fatal accidents caused by alcohol intoxication, as found in 1995 by Pack et al [2]. Additionally, there are a plethora of adverse health outcomes that result from chronic sleep deprivation, such as increased pain sensitivity [3-6] and impairments in endocrine, metabolic, and cardiac function, consequentially increasing the risk of type II diabetes [7,8], obesity [8], high blood pressure [7,9], and cardiovascular disease [7,9].
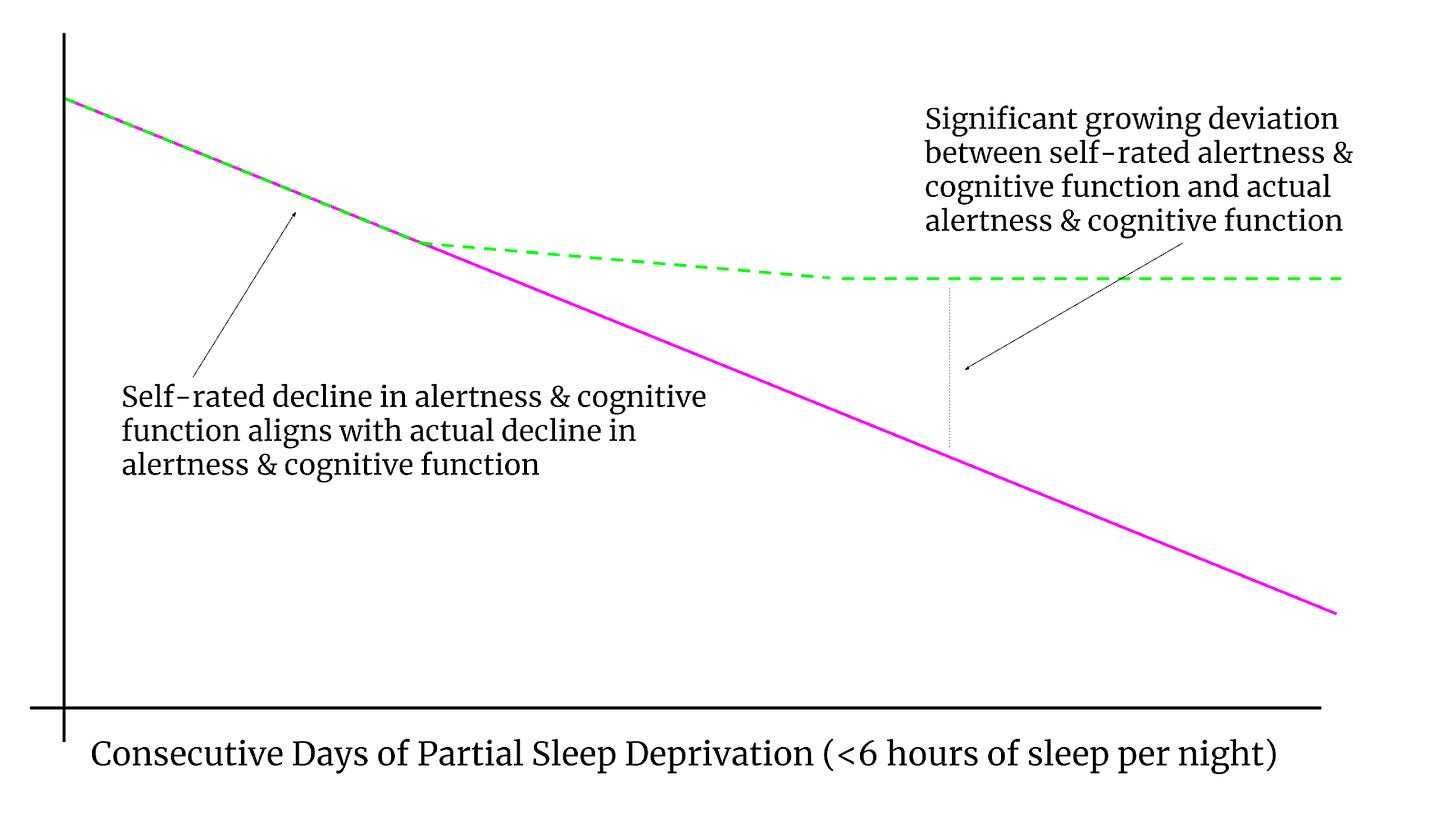
Again, “change is more perceptible than magnitude”. Similar to how we physically perceive the propulsion of an airplane most during take off (the period of the greatest change in speed), we perceive our own psychomotor and cognitive deficiencies most in the first few days of going from well-slept to poorly-slept. Then, similar to how we don’t physically perceive the propulsion of an airplane at the much faster cruising altitude (the period of constant velocity), we fail to perceive our gradual decline in psychomotor and cognitive ability when sleep deprived over the course of many consecutive days (i.e. a constant velocity of sleep deprivation). We often are only able to retrospectively realize that such impairments occurred after we are well-slept again, which is another period of change, but in the opposite direction, similar to the physically perceptible braking forces initiated by a plane during landing. Below is a simplified graph to demonstrate the difference between perceived decline in performance versus actual decline in performance.
This concept of “change is more perceptible than magnitude” can be applied endlessly in our own experience of health. When you’re feeling great, you often don’t realize how great you feel until you break a bone, injure your back, or get the flu. Conversely, we can go weeks, months, and even years experiencing a compromised level of health due to normalized, imperceptible dysfunction (i.e. constant velocity of dysfunction). The steadier and longer-lasting the dysfunction, the greater the likelihood the dysfunction is undetectable to our own senses. For more information on the difficulty of perceiving adverse health changes, check out this article.
Children in school often don’t realize how much they need corrective lenses until someone else realizes they can’t read the board. Individuals with chronic anxiety or depression can often fail to recognize the impact of their poor mental health until their psychological issues precipitate a crisis, or they begin getting treatment. Those with undiagnosed food allergies can often chronically experience gastrointestinal problems, headaches, and joint pain for decades, simply because they’ve eaten food they’ve been allergic to ever since they were a child, and they don’t know what it feels like to be well. It’s important not to underestimate the mind and body’s ability to normalize dysfunction. As a closing prompt: take time to deeply and honestly consider your daily experience of mental, emotional, and physical health. What constant velocities are you flying at, and are they moving you in the direction you want?
References
Van Dongen, H. P., Maislin, G., Mullington, J. M., & Dinges, D. F. (2003). The cumulative cost of additional wakefulness: dose-response effects on neurobehavioral functions and sleep physiology from chronic sleep restriction and total sleep deprivation. Sleep, 26(2), 117-126.
Pack, A. I., Pack, A. M., Rodgman, E., Cucchiara, A., Dinges, D. F., & Schwab, C. W. (1995). Characteristics of crashes attributed to the driver having fallen asleep. Accident Analysis & Prevention, 27(6), 769-775.
Kundermann, B., Spernal, J., Huber, M. T., Krieg, J. C., & Lautenbacher, S. (2004). Sleep deprivation affects thermal pain thresholds but not somatosensory thresholds in healthy volunteers. Psychosomatic Medicine, 66(6), 932-937.
Lautenbacher, S., Kundermann, B., & Krieg, J. C. (2006). Sleep deprivation and pain perception. Sleep Medicine Reviews, 10(5), 357-369.
Onen, S. H., Alloui, A., Gross, A., Eschallier, A., & Dubray, C. (2001). The effects of total sleep deprivation, selective sleep interruption and sleep recovery on pain tolerance thresholds in healthy subjects. Journal of Sleep Research, 10(1), 35-42.
Moldofsky, H. (2001). Sleep and pain. Sleep Medicine Reviews, 5(5), 385-396.
Spiegel, K., Leproult, R., & Van Cauter, E. (1999). Impact of sleep debt on metabolic and endocrine function. The Lancet, 354(9188), 1435-1439.
Knutson, K. L., Spiegel, K., Penev, P., & Van Cauter, E. (2007). The metabolic consequences of sleep deprivation. Sleep Medicine Reviews, 11(3), 163-178.
Mullington, J. M., Haack, M., Toth, M., Serrador, J. M., & Meier-Ewert, H. K. (2009). Cardiovascular, inflammatory, and metabolic consequences of sleep deprivation. Progress in Cardiovascular Diseases, 51(4), 294-302.